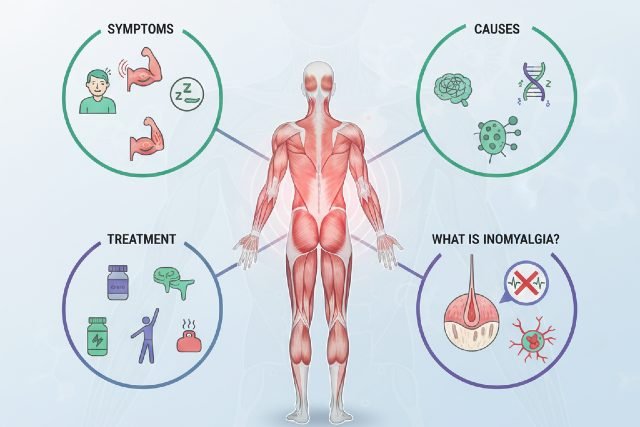
Inomyalgia is a term used to describe persistent muscle pain that cannot be explained by injury, infection, or common musculoskeletal disorders. Although the word may resemble similar terms like myalgia or fibromyalgia, inomyalgia stands as a broader descriptor for chronic muscle discomfort with unclear origins. Understanding inomyalgia is important because many people experience lingering muscle pain without receiving a clear diagnosis, and early recognition helps ensure proper evaluation and symptom management. In this guide, the keyword “inomyalgia” will be explored in depth by examining its symptoms, possible causes, diagnosis, and treatment options.
Understanding the Term “Inomyalgia”
The term combines “ino,” referring to muscle fibers, and “myalgia,” meaning muscle pain. Unlike conditions such as fibromyalgia, which is classified as a chronic widespread pain syndrome, inomyalgia focuses specifically on deep muscle discomfort that persists over time. Although not a medical diagnosis recognized in formal classification manuals, healthcare professionals use the term informally to describe certain pain patterns. This makes it important to distinguish inomyalgia from nerve pain, inflammatory disorders, and mechanical injuries so that treatment can be tailored appropriately.
Symptoms of Inomyalgia
People experiencing inomyalgia often report muscle tenderness that worsens with physical activity or stress. The pain may appear in one region or spread across multiple areas of the body. Some individuals describe a dull, aching sensation, while others report sharp pain during movement or palpation. The chronic nature of these symptoms can interfere with sleep, energy levels, and daily routines. Many individuals also mention morning stiffness, tension, and difficulty relaxing muscles, suggesting a possible link between stress and symptom intensity. Because these symptoms resemble those of other chronic pain disorders, proper evaluation is essential.
Commonly Overlapping Conditions
Although inomyalgia is discussed independently, it frequently overlaps with conditions such as chronic fatigue syndrome, fibromyalgia, and myofascial pain syndrome. Research from the National Institutes of Health shows that chronic pain conditions often coexist and share underlying mechanisms related to central sensitization. This means the nervous system becomes more sensitive to pain signals over time, causing normal sensations to feel uncomfortable or even painful. Understanding this overlap helps patients and clinicians consider comprehensive treatment approaches instead of focusing solely on muscle tissue.
Potential Causes of Inomyalgia
Because inomyalgia is not yet fully defined in clinical guidelines, its causes remain uncertain. However, several contributing factors have been identified through pain research and clinical observation. Muscle overuse is one possible trigger, especially in individuals who perform repetitive physical activities. Stress may also play a key role, as chronic stress increases the release of cortisol and other hormones that affect muscle tension. Some studies suggest that sleep disturbances contribute to muscle pain because the body repairs tissues during deep sleep. When this process is disrupted, muscles may feel fatigued or tender.
Another potential factor is nutritional imbalance. Deficiencies in vitamin D, magnesium, or potassium are known to contribute to muscle pain. Although this does not directly cause inomyalgia, correcting these deficiencies may reduce symptom severity. Lastly, underlying health conditions such as thyroid disorders, autoimmune diseases, and viral infections could produce similar symptoms, which is why medical evaluation is necessary before assuming the pain is due to inomyalgia alone.
How Inomyalgia Is Diagnosed
Since inomyalgia is not a formal medical diagnosis, healthcare providers instead rule out other causes of chronic muscle pain. This process may include physical examinations, blood tests, imaging studies, and assessments of lifestyle and stress levels. The goal is to identify any underlying condition that may explain the symptoms. If none are found, clinicians may use the term inomyalgia to describe a chronic pain pattern that requires symptomatic treatment. This form of diagnosis relies heavily on patient history, making accurate and detailed reporting essential.
Treatment Options for Inomyalgia
Treatment for inomyalgia focuses on reducing pain, improving muscle function, and enhancing quality of life. Physical therapy is commonly recommended because it helps strengthen muscles, improve posture, and reduce tension. Gentle stretching and low-impact exercises, such as yoga, can also be beneficial. Some patients find relief through massage therapy and heat application, which help relax tight muscles.
Stress management plays a major role in symptom control. Techniques such as mindfulness meditation, deep breathing, and cognitive-behavioral therapy can help regulate the body’s response to stress. Research from the American Psychological Association highlights how psychological stress significantly influences muscle tension and pain perception, supporting the value of mind-body approaches.
Sleep improvement strategies may include setting consistent bedtimes, reducing screen time before sleep, and creating a peaceful sleep environment. Quality sleep supports muscle recovery and reduces sensitivity to pain. In some cases, healthcare providers may recommend medications such as anti-inflammatory drugs or muscle relaxants, although these are typically used short-term.
Because nutritional imbalances may contribute to muscle discomfort, healthcare professionals sometimes recommend dietary adjustments or supplements. Any supplements should be discussed with a medical provider, as individual needs vary widely.
Living With Inomyalgia: Real-World Insights
Living with inomyalgia can be challenging, particularly when the pain interferes with work, relationships, and daily responsibilities. Individuals often describe a cycle in which pain leads to reduced activity, which then worsens stiffness and discomfort. Breaking this cycle requires consistent management strategies and a supportive healthcare team. People who take a proactive approach — tracking symptoms, maintaining physical activity within comfortable limits, and managing stress — often report better outcomes.
One example involves individuals who experience muscle pain after long hours of desk work. By improving ergonomic setups and incorporating short movement breaks throughout the day, many people notice significant improvements. Another example is athletes who develop persistent muscle soreness despite adequate training. Identifying overtraining patterns, adjusting routines, and focusing on recovery techniques can make a noticeable difference.
Frequently Asked Questions
Is inomyalgia the same as fibromyalgia?
No. Fibromyalgia is a clinically recognized condition characterized by widespread pain, fatigue, and additional symptoms such as cognitive difficulties. Inomyalgia refers specifically to chronic muscle pain without a clear diagnosis and does not encompass the full spectrum of fibromyalgia symptoms.
Can inomyalgia go away on its own?
Symptoms may improve with lifestyle changes, stress reduction, and consistent physical activity. However, chronic pain patterns often require ongoing management rather than expecting a complete and permanent resolution.
Should I see a doctor for muscle pain?
Yes. Because many medical conditions can cause muscle pain, professional evaluation is important before assuming the pain is due to inomyalgia.
Conclusion
Inomyalgia represents a form of persistent muscle pain that lacks a clearly identifiable cause, yet significantly affects daily life. Understanding the symptoms, potential triggers, and available treatment approaches can help individuals take control of their health. Whether the pain is due to stress, overuse, nutritional factors, or other underlying issues, early evaluation and a comprehensive management plan are essential. By adopting supportive strategies and working with qualified healthcare professionals, many people find meaningful relief and improved well-being. This guide highlights the key aspects of inomyalgia to promote greater awareness and encourage proactive care.